Tips For Applying A Pelvic Binder
Applying a pelvic binder is a critical skill for healthcare providers in managing patients with pelvic fractures or unstable pelvic injuries. A pelvic binder is a device used to stabilize the pelvis, reducing bleeding, pain, and the risk of further injury. In this guide, we will provide you with tips for applying a pelvic binder effectively and safely.
Assess the patient's condition: Before applying a pelvic
binder, it is crucial to assess the patient's overall condition. Ensure that
the patient's airway, breathing, and circulation are stable. If there are any
immediate life-threatening injuries, address them first.
Gather necessary equipment: Collect all the equipment
required for applying a pelvic binder. This typically includes a pelvic binder device, gloves, trauma shears, and tape. Ensure that all equipment is readily
accessible.
Communicate with the patient: Explain the procedure to the
patient and obtain their consent. Reassure the patient and tale any concerns
they may have. Maintain a calm and reassuring demeanor throughout the process.
Position the patient: Position the patient supine on a firm
surface. Ensure their legs are extended and straight. The patient's feet should
be flat on the surface, and the knees should be slightly bent.
Expose the patient's pelvis: Use trauma shears to carefully
remove or cut through the patient's clothing to expose the pelvic region. Be
cautious not to cause additional harm or discomfort to the patient.
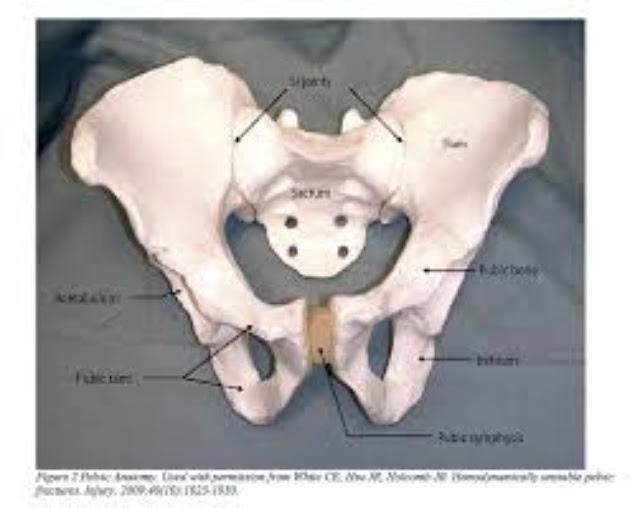
Assess for bony landmarks: Locate the bony landmarks on the patient's pelvis. The anterior superior iliac vertebral column (ASIS) and pubic symphysis are commonly used as reference points for applying a pelvic binder.
Apply the binder: Position the pelvic binder device over the
patient's pelvis, aligning it with the ASIS on each side. Ensure that the
binder is centered over the pubic symphysis. The binder should be snug but not
overly tight, allowing for adequate stabilization without compromising blood
flow or causing unnecessary discomfort.
Secure the binder: Fasten the pelvic binder securely. Trail
the manufacturer's instructions for the specific device being used. Typically,
this involves tightening straps or using Velcro closures to secure the binder
in place.
Reassess and monitor: Once the pelvic binder is applied,
reassess the patient's vital signs and overall condition. Monitor for any signs
of worsening pain, decreased blood flow, or other complications. Make necessary
adjustments to the binder if needed.
Immobilize the patient: Consider additional measures to
immobilize the patient and prevent further movement. This may involve placing a
cervical collar, using a backboard, or utilizing other spinal immobilization
techniques, depending on the patient's overall condition and suspected
injuries.
Transport the patient: Arrange for timely transportation of
the patient to a medical facility equipped to manage pelvic injuries.
Communicate with the receiving facility to provide them with relevant
information about the patient's condition and the application of the pelvic
binder.
Document the procedure: Thoroughly document the procedure, including the time of application, any adjustments made, and the patient's response. This documentation is essential for accurate communication, ongoing care, and medicolegal purposes.
Continuously reassess the patient: Throughout the patient's
care, continue to reassess their condition regularly. Monitor vital signs,
neurovascular status, and pain levels. Adjust the pelvic binder or consider
alternative interventions if the patient's condition changes or deteriorates.
Seek expert consultation if needed: If you encounter
challenges or complexities in managing the patient's pelvic injury, don't
hesitate to seek expert consultation. Reach out to a trauma surgeon, orthopedic
specialist, or another healthcare professional experienced in managing pelvic
fractures.
Ongoing education and training: Keep yourself updated with
the latest guidelines and recommendations for managing pelvic injuries.
Participate in relevant training programs and simulations to enhance your
skills and confidence in applying a pelvic binder.
Remember, the application of a pelvic binder should be done by trained healthcare providers. These tips are meant to provide general guidance but should not replace formal training or clinical judgment. Always follow your organization's protocols and seek appropriate supervision and assistance when necessary.


